Hospital medical liability in Portland presents real challenges for healthcare facilities. Claims are rising, regulations are tightening, and the financial stakes are high. This guide walks you through the risks you face, the coverage options available, and the practical steps to strengthen your defenses.
What Liability Risks Do Portland Hospitals Face?
Misdiagnosis, surgical errors, and hospital-acquired infections dominate malpractice claims in Portland. Misdiagnosis claims require proving that a provider deviated from the standard of care and that delayed or wrong treatment caused harm. Surgical errors cover wrong-site procedures, retained instruments, and operative mistakes — all requiring strong evidence of negligence. Infections and sanitation failures represent the third major category, where hospitals face liability for conditions that harm patients.

In 2023, Oregon physicians alone faced 94 medical malpractice payouts totaling about $70.4 million, according to the National Practitioner Data Bank, with an average payout of roughly $748,909 per claim. The standard of care in Oregon is defined by statute as the care, skill, and diligence of ordinarily careful physicians in similar circumstances. Proving breach requires testimony from a qualified expert in the same medical field, making these cases expensive and complex from the start.
Oregon’s Two-Year Window and Five-Year Deadline
Time matters enormously in Portland hospital liability. Oregon’s statute of limitations gives patients two years from when they discovered malpractice, or should have discovered it, to file a claim. However, an absolute deadline of five years from the date of treatment applies regardless of discovery, with limited exceptions for fraud. This means hospitals must preserve all records and communications carefully, and staff must document everything thoroughly.
Communication lapses, medication mistakes, and failures to follow up trigger many claims. Oregon has no cap on non-economic damages in personal injury cases, which means pain, suffering, and emotional distress can drive settlements and verdicts significantly higher than medical costs alone. Wrongful death cases cap non-economic damages at $500,000, but economic damages have no ceiling. This absence of damage caps distinguishes Oregon from many other states and increases financial exposure for Portland hospitals.
Premium Costs and Reinsurance Pressure
Medical liability premiums in Oregon rose sharply in 2020, with a 16.7% increase driven by claim severity and reinsurance costs, according to analysis of Medical Liability Monitor data. Nationally, year-over-year premium increases hit 31.1% in that period, the highest rate since 2005. Payout size matters more than claim frequency for pricing, meaning one high-severity lawsuit pushes costs higher across the entire facility.
Reinsurance costs act as a primary driver of rising premiums; when reinsurers raise rates, those costs transmit directly to hospital policies. The Portland metro market has experienced contractions in insurer competition, limiting your options for coverage and pricing leverage. The main Oregon carriers writing medical liability include The Doctors Company, MedPro Group, and CNA (all with AM Best A-level or higher ratings), though carrier appetite varies by specialty and practice size. Shopping across multiple carriers via a broker can save 20% or more versus staying with a single carrier, making competitive quotes essential before renewal.
Understanding these risks sets the stage for evaluating the coverage options that actually protect your facility.
Coverage Structures That Protect Your Portland Hospital
Hospital medical liability coverage splits into distinct layers and selecting the wrong structure can cost thousands annually. General liability policies cover bodily injury and property damage from non-professional acts. For example, a patient slips in a hallway, or someone sustains injury from facility conditions. Professional liability insurance covers the clinical decisions themselves: misdiagnosis, surgical errors, medication mistakes, and failures in care. Portland hospitals need both, but they operate separately and carry different limits. Most facilities carry $1 million per claim and $3 million aggregate limits, though some hospitals demand higher thresholds depending on facility size and risk profile.
Selecting Your Carriers and Limits
The Doctors Company, MedPro Group, and CNA remain the primary Oregon carriers with strong AM Best ratings, but their appetite for specific specialties and practice sizes varies considerably. Shopping quotes across multiple carriers through a broker consistently saves 20% or more compared to renewing with a single insurer. This isn’t optional if you want competitive pricing in Portland’s tightening market. You’ll find that carrier appetite shifts based on your facility’s claims history, specialty mix, and patient volume, so annual shopping prevents you from overpaying.
Claims-Made Versus Occurrence: The Financial Trade-Off
Claims-made policies versus occurrence policies represent the second critical decision, and the math shifts based on your practice timeline. Claims-made policies carry lower upfront premiums but require tail coverage when you retire or leave Oregon; tail policies typically cost 40–60% more annually than your base premium, sometimes doubling your final-year costs. Occurrence policies cost 40–60% more each year but eliminate the tail requirement entirely — you pay more upfront but walk away clean. If you plan a long-term practice in Portland, claims-made with tail coverage often make financial sense over ten-plus years.

If retirement or relocation happens within five years, occurrence policies shift the calculation toward better value.
Hospital-Specific Coverage Requirements
Specialized hospital coverage includes vicarious liability (the hospital’s responsibility for employed physicians and independent contractors who appear to work for the facility), coverage for related services like radiology and pathology, and protection against regulatory investigations. Risk management programs that emphasize credentialing, clear documentation protocols, verified patient consent, and EHR safety checks reduce premiums by approximately 5–10% through most carriers. Facility terms with hospitals are negotiable — you don’t have to accept statutory minimums, and early conversations with risk management about exact coverage requirements before accepting a position prevent costly surprises later.
Understanding your coverage structure positions you to implement the risk management strategies that actually lower your exposure and protect patient safety.
How Documentation and Training Reduce Liability Exposure
Documentation as Your Primary Defense
Hospitals that treat documentation as a liability defense rather than an administrative burden see measurably lower claim rates. The standard of care in Oregon requires ordinarily careful physicians to document clinical reasoning, test results, and treatment decisions contemporaneously, not weeks later. When a claim arises, your medical records become the primary evidence of whether care met the standard. Incomplete notes, missing test results, or vague descriptions of patient interactions signal negligence to plaintiff attorneys and juries, even when care was appropriate.
Each provider should document the patient’s presenting complaint, physical examination findings, differential diagnoses considered, tests ordered and their results, treatment decisions, and patient instructions with specific dates and times. When medication errors occur, documentation showing verification steps, patient allergies reviewed, and dosage calculations checked demonstrate risk awareness. Electronic health records with hard stops for missing fields, required co-signatures for critical results, and automated alerts for abnormal findings prevent gaps that grow into claims.
Closing Communication Gaps That Trigger Claims
Communication failures trigger many claims — a radiologist spots an abnormality but fails to notify the ordering physician, or a nurse documents a concerning symptom without escalating to the attending. Your documentation system must require explicit signoffs confirming that critical information reached the right provider. Staff training on documentation standards should happen quarterly, not annually, with real examples from your facility’s own near-misses and resolved claims so providers see why specificity matters. Comprehensive documentation as part of safe patient care recognizes that detailed records protect both patients and the institution.
Credentialing and Staff Training Lower Premium Costs
Credentialing and staff training directly reduce premium costs because carriers recognize that disciplined hiring and ongoing education lower claim severity and frequency. The Doctors Company, MedPro Group, and CNA all offer risk management credits of approximately 5–10% when hospitals implement credentialing verification, malpractice prevention training, clear handoff protocols, detailed documentation audits, verified patient consent procedures, and EHR safety checks.
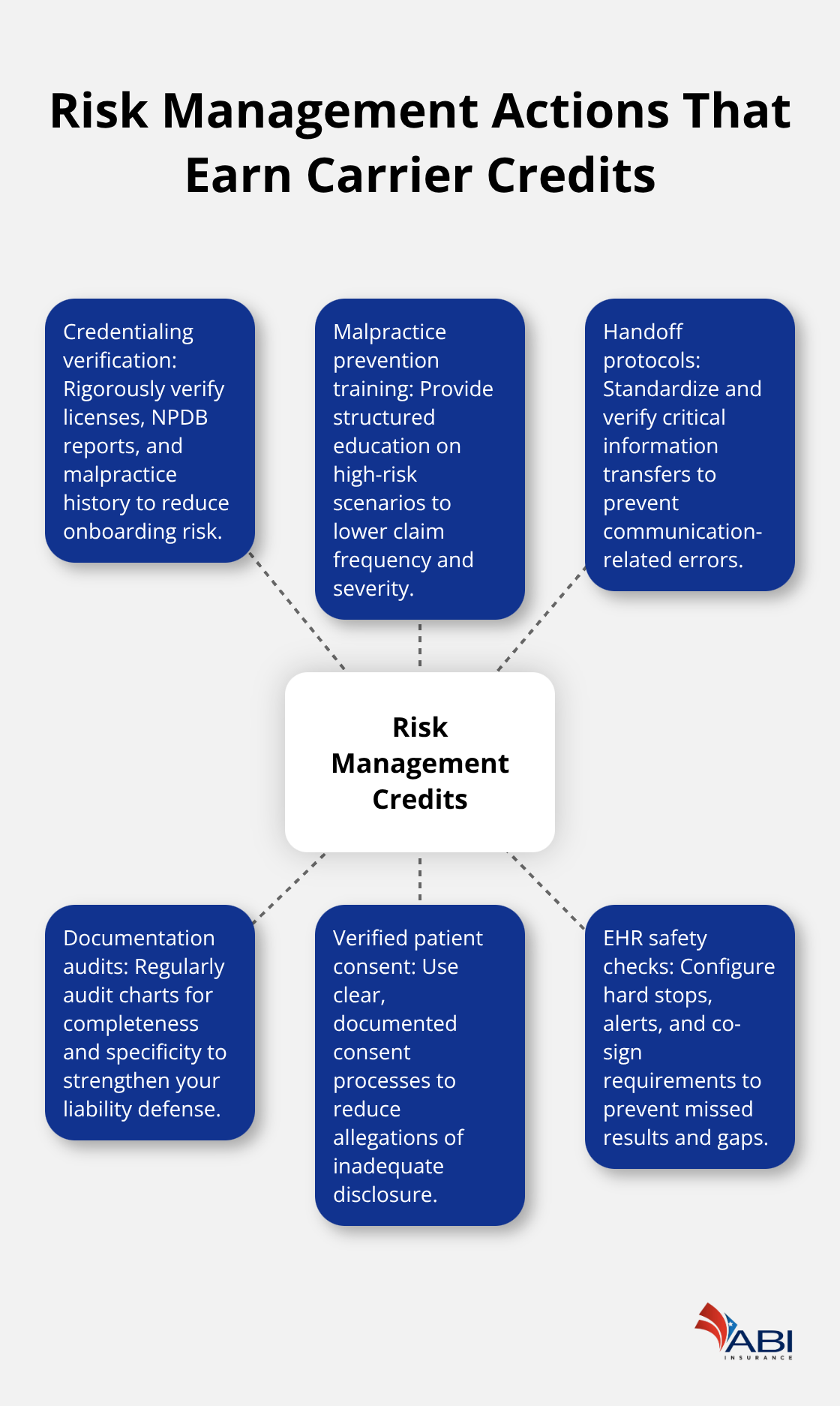
Portland hospitals should credential all physicians and advanced practice providers against the National Practitioner Data Bank, verify licenses with the Oregon Medical Board, and check malpractice history before appointment. Recredentialing every two years catches license suspensions, new claims, and practice restrictions before they become institutional liability. Staff training programs addressing medication safety, surgical site verification, handoff communication, and infection control should be mandatory and documented. When new staff join, assign mentorship from experienced providers and verify competency in high-risk procedures before independent practice.
Measuring Safety Culture Through Quality Assurance
Patient safety committees that meet monthly review adverse events, near-misses, and claims trends to identify systemic problems before they cause harm to multiple patients. Quality assurance programs measuring infection rates, readmission rates, and patient satisfaction provide early warning of deteriorating safety culture. These metrics also demonstrate to carriers that your facility takes risk seriously, justifying lower premiums and better coverage terms. Risk management training that covers informed consent, communication protocols, and early recognition of deteriorating patients saves lives and prevents lawsuits.
Final Thoughts
Hospital medical liability in Portland demands action across three fronts: understand your risks, select coverage that matches your exposure, and build a safety culture that prevents claims before they start. The 2023 data showing $70.4 million in Oregon payouts across 94 claims underscores why half-measures fail. Your facility faces real financial exposure, especially with Oregon’s uncapped non-economic damages and the five-year absolute deadline for claims.
Claims-made policies with tail coverage, occurrence policies, or a hybrid approach each carry different financial implications depending on your practice timeline and facility size. Shopping across The Doctors Company, MedPro Group, and CNA through a broker saves 20% or more annually compared to single-carrier renewal. Risk management delivers measurable returns — documentation standards, credentialing verification, staff training, and quality assurance programs reduce premiums by 5–10% while lowering claim severity and frequency.
When your staff documents clinical reasoning contemporaneously, communicates critical findings explicitly, and follows verified handoff protocols, you prevent the communication lapses and medication errors that dominate malpractice claims. Contact ABI Insurance to evaluate your current coverage, compare quotes across multiple carriers, and implement risk management practices that strengthen your defenses against hospital medical liability in Portland. The time to act is now, before the next claim arrives.












 Portland BOP Quotes: Comparing Coverage for Local Businesses
Portland BOP Quotes: Comparing Coverage for Local Businesses







